
Powered By





If you’ve noticed colored patches or spots on your skin, you may have a condition called purpura. These spots show up when small blood vessels leak under the skin. Purpura can affect people with Sjögren’s disease, but it can also happen with other medical conditions.
About half of the people with Sjögren’s disease experience skin symptoms. Dry skin and itchy rashes are common issues. Some people also develop different types of bumps and discolored spots. Your healthcare provider will need to see you in person to figure out what’s causing your symptoms.
Here’s what could be causing those red or brown spots on your skin and what you should do about them.
Purpura is the medical term for blood spots on the skin. They may appear as little dots or patchy areas. These spots are usually between 4 and 10 millimeters wide. Smaller spots are called petechiae. Larger spots are considered bruises.
Just under the skin’s surface is a network of tiny blood vessels. Some conditions cause the blood vessels to become irritated and swollen. As a result, these delicate vessels may burst open and leak some blood, leading to purpura.
Purpura isn’t a standalone condition. It’s a symptom of something else. Some people develop purpura because of a medication they’re taking or a vitamin deficiency (such as vitamin C). Others have an underlying disease that puts them at risk for purpura, like Sjögren’s disease.
Possible causes of purpura include:
Purpura can show up anywhere on the body, including the mucous membranes and inside of the mouth. You’ll often see them on your arms and hands or your legs and feet.
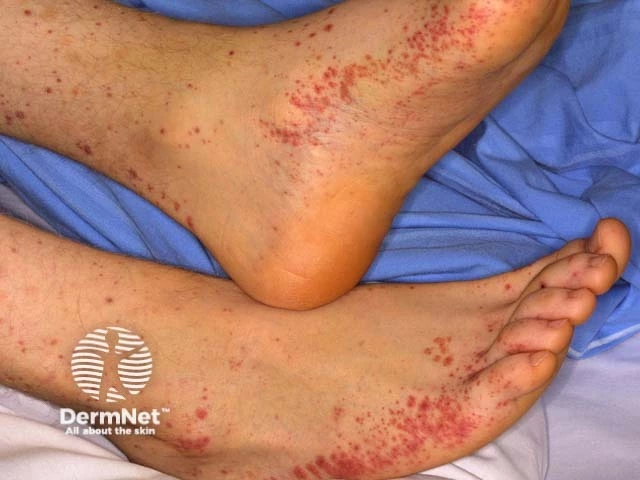
Skin with purpura may feel a little tender, but purpura itself usually isn’t very painful or itchy. Purpura can be flat or raised. Raised purpura is common with inflamed blood vessels (vasculitis). Flat purpura is more often seen with low platelets or blood-clotting problems. In addition, purpura doesn’t disappear when you press on your skin.
There are a few different reasons that people with Sjögren’s may develop purpura. It can be directly related to Sjögren’s or another issue entirely.
People with Sjögren’s are prone to vasculitis. Vasculitis means inflammation of the blood vessels. It’s one of the main causes of purpura in Sjögren’s disease.
Vasculitis can be a temporary issue or a long-lasting problem. It may come with other symptoms such as:
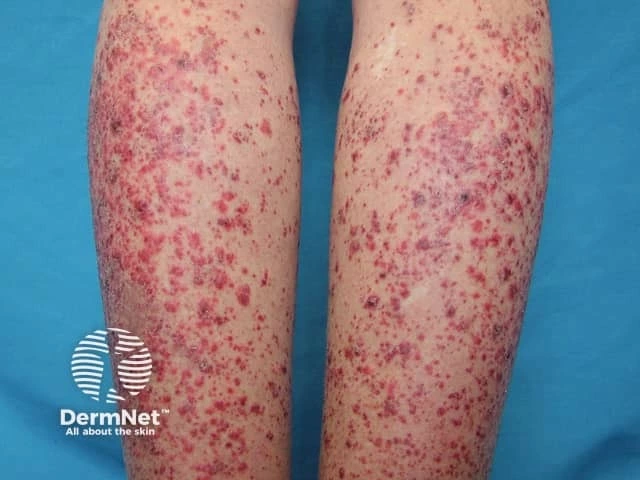
These symptoms may worsen or flare at certain times, then improve. Vasculitis can affect any organ of the body. When it affects the skin, the symptoms can be more severe than purpura. Bigger lesions, lumps, or sores can also develop.
People who have one autoimmune disease (like Sjögren’s) have a higher chance of developing another autoimmune condition. Autoimmune diseases happen when the immune system mistakenly attacks the body’s own healthy tissues. Many autoimmune diseases affect the skin. For instance, cutaneous lupus and psoriasis are autoimmune conditions that cause skin symptoms. Part of your diagnosis will likely include ruling out other skin conditions.
Low platelet counts can also cause purpura. Sometimes people with Sjögren’s develop a secondary autoimmune condition called immune thrombocytopenia (ITP). ITP affects platelets and leads to symptoms like purpura and bruising.
Purpura is a common condition. It can happen in people of all ages. Sometimes purpura goes away on its own without treatment, but it’s always a good idea to let your doctor know if you see any changes in your skin. Even if purpura doesn’t hurt, it can still be a sign of a health problem that needs medical care.
Most purpura in Sjögren’s involves small blood vessels in the skin and does not affect larger blood vessels. If your doctor thinks a larger blood vessel problem is possible based on your symptoms, they may order special imaging tests. Surgery is not usually needed for Sjögren’s-related skin purpura.
Since Sjögren’s can increase the chance of various skin issues, your doctor will need to examine your skin to see if the issue is truly purpura or something else. Be sure to tell them about any medications or supplements you take, as these could be related to your skin problems.
Your healthcare provider will ask when your purpura symptoms started. Try to share as much information as you can, including any lifestyle changes you’ve made or other symptoms you’ve been having. Your provider will also review your medical history and may order tests to find the cause.
Different specialists can help you find the answers you’re looking for. A rheumatologist can manage the autoimmune aspects of Sjögren’s, including checking for other autoimmune diseases that can be responsible for skin symptoms. They may refer you to a dermatologist for testing or guidance on skin care.
Testing may involve a blood test to check your platelet counts and a skin biopsy. During a skin biopsy, a small sample of skin is removed and sent to a lab for testing. If you have vasculitis, you may need imaging tests like X-rays, ultrasounds, CT scans, and MRIs.
There are several ways to treat purpura, depending on what’s causing it. The first step will be to address the underlying cause. Your healthcare provider may also advise changing your medications or trying practical steps, like covering the spots with clothing or makeup, to help you feel more comfortable while you treat the cause.
If you have low platelets, your doctor may recommend corticosteroids to help prevent platelet destruction. They may also recommend intravenous immunoglobulin or a platelet transfusion for a short-term boost. Platelet transfusions are usually saved for serious bleeding or urgent procedures.
Immunosuppressant medications or therapies called thrombopoietin receptor agonists may help your body keep platelet counts higher. Lowering inflammation can also help treat vasculitis. In some cases, removing the spleen may be an option, but it isn’t right for everyone. Your healthcare provider can help you weigh the benefits and risks based on your symptoms and test results.
On MySjögrensTeam, people share their experiences with Sjögren’s disease, get advice, and find support from others who understand.
How has Sjögren’s affected your skin? Let others know in the comments below.
Get updates directly to your inbox.



Become a member to get even more




This is a member-feature!
Sign up for free to view article comments.
After I had sepsis in October 2021 then both arms (but the left more) showed purpura on my lower arms. Never went away and now I’m getting a few spots on upper arms. I use aqua pur ointment and… read more
We'd love to hear from you! Please share your name and email to post and read comments.
You'll also get the latest articles directly to your inbox.